Chronic joint and tendon pain can quietly reshape everyday life. Tasks that once felt simple, such as climbing stairs, carrying groceries, or exercising, may begin to feel uncomfortable or exhausting. These conditions often develop gradually as inflammation builds in the joints or connective tissues. Over time, this irritation can reduce mobility and make people hesitant to stay active. When movement decreases, stiffness and weakness can increase, which creates a frustrating cycle for many patients.
For years, many people believed surgery was the only dependable solution for serious joint or tendon problems. Surgery can be effective in some situations, but it is not always the first or only option. Medical research now focuses heavily on treatments that help the body repair damaged tissue without invasive procedures. These methods aim to manage inflammation while supporting natural healing, helping patients regain movement and comfort.
Why Persistent Inflammation Makes Joint and Tendon Pain Hard to Treat
Inflammation plays an important role in the body’s healing process. When tendons or joints are stressed by injury, overuse, or strain, the immune system responds with inflammation to initiate tissue repair. In many cases, this response works well. The tissue heals, and pain gradually disappears. However, when irritation persists or healing slows, inflammation can persist much longer than expected.
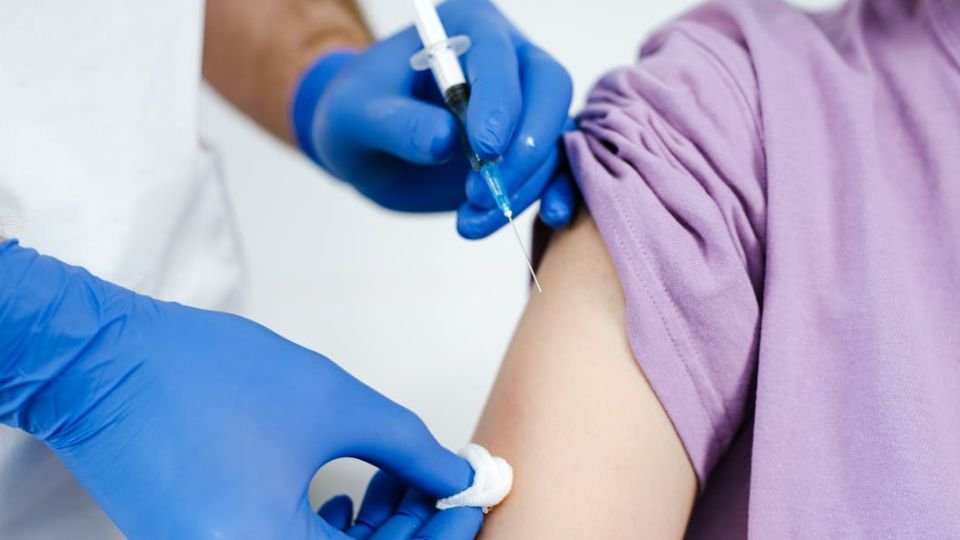
Long-term inflammation can keep tissues in a constant state of irritation. Basic treatments such as rest, ice, and anti-inflammatory medication may reduce symptoms temporarily but often fail to repair damaged tissue. When pain continues, physicians may explore regenerative options that target healing directly. One example is PRP treatment, which uses concentrated components from a patient’s own blood to stimulate repair and help calm persistent inflammation in injured tendons or joints.
Understanding the Science Behind Regenerative Medicine
Regenerative medicine focuses on improving the body’s natural ability to repair damaged tissue. Instead of replacing injured structures with artificial materials, these treatments encourage the body to rebuild its own cells and connective tissue. Doctors use biological components that support healing signals within the injured area, helping restore normal tissue function.
This process relies on the body’s built-in repair system. Cells release proteins and growth factors that guide the rebuilding of tissue and support healthy blood circulation. When these biological signals are concentrated and delivered directly to the injured site, they can promote tissue repair in tissues that have struggled to heal on their own.
Common Causes of Tendonitis and Joint Degeneration
Tendonitis and joint degeneration often develop from repeated physical stress. Athletes, manual laborers, and people with demanding physical routines often strain specific joints or tendons. Over time, small microscopic injuries accumulate in these areas. When the body cannot fully repair these injuries between activities, inflammation builds, and pain gradually increases.
Age also contributes to joint and tendon problems. As the body ages, connective tissues lose some elasticity, and cartilage becomes thinner. Previous injuries can also weaken a joint and change how the body distributes pressure during movement. These changes make certain areas more vulnerable to inflammation and long-term degeneration.
Cortisone Injections vs Regenerative Therapies
Cortisone injections are commonly used to reduce inflammation in painful joints and tendons. The medication suppresses inflammatory signals in the affected area, which can quickly reduce swelling and discomfort. Many patients experience noticeable relief within a short time. This makes cortisone helpful for temporary symptom control.
However, cortisone primarily reduces inflammation rather than repairing damaged tissue. In some situations, repeated injections may weaken surrounding structures over time. Regenerative therapies approach the problem differently. These treatments encourage the body to repair injured tissue and strengthen the affected area, which may lead to longer-lasting improvement in joint and tendon health.
How Blood-Derived Growth Factors Help Accelerate Tissue Repair
Blood contains platelets that play an important role in healing after injury. These platelets release growth factors that signal nearby cells to begin repairing damaged tissue. When a tendon or ligament is injured, the body naturally sends these signals, but sometimes the response is slow or limited. Concentrating these healing elements allows doctors to deliver a stronger repair signal directly to the injured area.
This targeted approach encourages tissue regeneration where it is needed most. Growth factors can stimulate collagen production and support the rebuilding of connective tissue. As healing improves, inflammation may decrease, and joint stability can improve. For many patients, this process supports recovery without the need for invasive procedures.
Lifestyle Habits That Support Stronger Joints and Tendons
Daily habits strongly influence joint and tendon health. A balanced diet that includes omega-3 fatty acids, lean protein, and vitamin-rich foods can help control inflammation and support tissue repair. Nutrients such as vitamin C and magnesium also play a role in collagen formation, which keeps connective tissues strong and flexible.
Regular movement is equally important. Low-impact activities such as swimming, cycling, and walking strengthen muscles that stabilize joints. Maintaining a healthy body weight also reduces pressure on weight-bearing joints, such as the knees and hips. Over time, these habits help protect joints from additional strain and support long-term mobility.
The Role of Physical Therapy in Long-Term Recovery
Physical therapy plays a central role in managing joint and tendon pain. A therapist evaluates movement patterns and identifies areas of weakness or imbalance that may contribute to injury. Through guided exercises, patients gradually strengthen surrounding muscles and improve joint stability.
Therapy also focuses on flexibility and controlled movement. Stretching routines and mobility exercises can improve the range of motion and reduce stiffness in affected joints. When patients follow a structured rehabilitation program, they often experience better function and a lower risk of reinjury during everyday activities.
When to Seek Professional Medical Evaluation
Some joint or tendon pain improves with rest and basic home care. However, persistent symptoms may signal a deeper issue that requires medical evaluation. Pain that lasts for several weeks, swelling that does not improve, or difficulty moving a joint should prompt a consultation with a healthcare professional.
Early assessment can prevent small injuries from becoming chronic problems. Doctors may recommend imaging, targeted therapy, or regenerative treatments depending on the condition. Addressing the problem early allows patients to explore non-surgical options and begin a treatment plan that supports recovery and long-term joint health.